Earlier this year, New Market firefighter–EMT Kourtney Minton responded to two 911 calls in two months from two Exxon gas stations in the small Shenandoah County town.
Both calls came from women in labor who had to pull over while making the 45-minute drive from their homes in Page County over Massanutten Mountain and on to Harrisonburg’s Sentara RMH Medical Center to give birth.
“The first one that we had, she was coming from home, trying to get to Sentara; that was the plan,” Minton said. “She delivered in the Exxon parking lot prior to our arrival.”
Minton delivered the second baby herself in the back of an ambulance while they raced south on Interstate 81 toward Harrisonburg.
“The first cry is a sigh of relief, you know the baby's OK because they're crying,” she said. “The baby's crying, mom's crying because she just delivered her little bundle of joy and I'm over here trying not to cry because I just delivered her little bundle of joy.”

There were 3,667,758 babies born in the U.S. in 2022, the most recent year for which U.S. Centers for Disease Control and Prevention birth data is available. All but 83,007 of them were born in hospitals.
But within the “In hospital” category, an unknown number of births that actually occurred “en route to or on arrival at hospital” are also included.
Page County has a population of less than 25,000, including only 3,889 women ages 15–44 — a range that research and advocacy nonprofit March of Dimes classifies as “childbearing age.”
That one EMT, one county over, would have two experiences like that in two months is part coincidence and part reflection of the reality that Page County is the epicenter of one of Virginia’s most severe maternity care deserts.
A maternity care desert is a county where there are no obstetric hospitals or birth centers, and no obstetric providers.
The CDC and Virginia Department of Health don’t release data about how many births happen on the way to a hospital or where they occur. But, in addition to the two Minton encountered, Sentara and a local midwifery practice confirmed a handful of car births in the region.
VPM News/WMRA has been investigating the lack of access to maternity care in the county and its dramatic impacts on pregnant people there.
The results are based on the most recent county, state and federal data, as well as interviews with more than a dozen people — including four Page County moms, four labor and delivery unit nurses and Virginia’s top maternal mortality researcher.
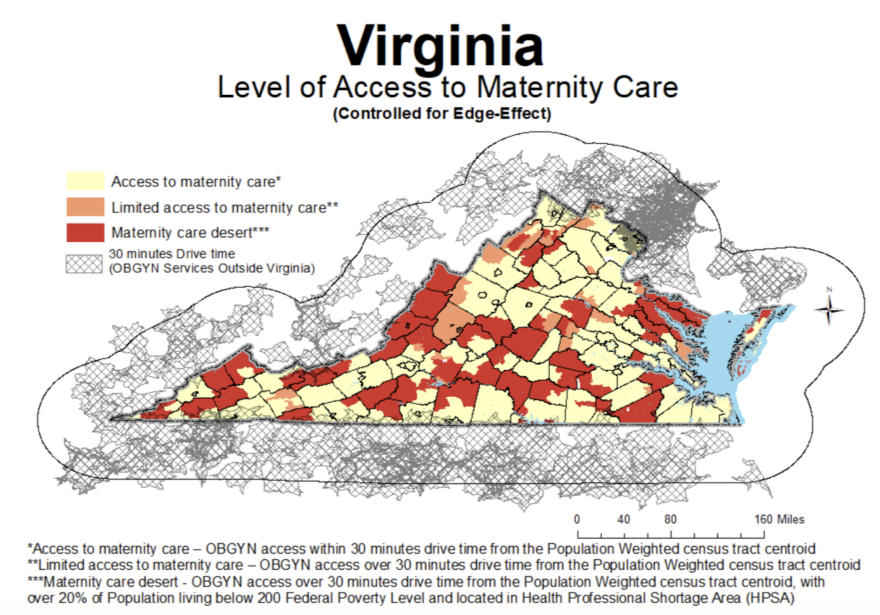
Being pregnant in a maternity care desert
Wedged between Massanutten Mountain and the Blue Ridge Mountains, Page County is a valley within the larger Shenandoah Valley.
The county has experienced significant change in recent decades as people have moved to Virginia’s “Cabin Capital” and driven up median income and housing costs in the process. But the area’s geography has ensured relative isolation.
While only just over Massanutten to the west, Shenandoah County has Interstate 81 — and the traffic, population and infrastructure that come with tens of thousands of people passing through each day.
Page County has the South Fork Shenandoah River as it winds through the county in neat switchbacks on its way to meet the Potomac in Harpers Ferry, West Virginia.

Colleen Cassidy lives in Rileyville, an unincorporated town of less than 1,000 people, just off one of the river bends.
“It's gorgeous out here. I stare at the mountain right out of my kitchen window. People are really nice,” she said. “It's just nice living out here. I don't have a single complaint living here, outside of being pregnant out here.”
Cassidy, a server recently turned stay-at-home mom, and her boyfriend, John Wallace, an electrician, bought their house about a year ago. Their move came shortly after she found out she was pregnant with her third child.
She quickly started looking for an OB/GYN in Page County but found “there wasn't anything around,” she said.
Historically, the closest labor and delivery unit — at Warren Memorial Hospital’s old campus in Front Royal — was less than 30 minutes from her. But when Valley Health, the dominant health system in the northern Shenandoah Valley, closed the unit about six years earlier in 2018, people like Cassidy were left with no good options:
- Winchester Medical Center, nearly an hour away, is the next closest unit to her.
- L&D units at Sentara in Harrisonburg, Fauquier Health in Warrenton and the University of Virginia’s Culpeper Medical Center are all also an hour away.
- UVA Health in Charlottesville and Augusta Health, outside of Staunton, are more than an hour away.
That distance, coupled with the fact there are no practicing OB/GYNs in the county, makes Page County a maternity care desert according to the most recent report from March of Dimes.
Cassidy chose Winchester Medical Center. But, worried about finding child care for her other children before the hour-long trip for delivery — or the possibility of a snowstorm trapping them at home — she scheduled a labor induction.
“[My boyfriend] works two hours from home, and we're an hour from the hospital. If I went into labor, I would have to wait for him to come home and then drive an hour to the hospital,” she said. “I was more concerned of not making it to the hospital — each baby, they say, gets quicker.”
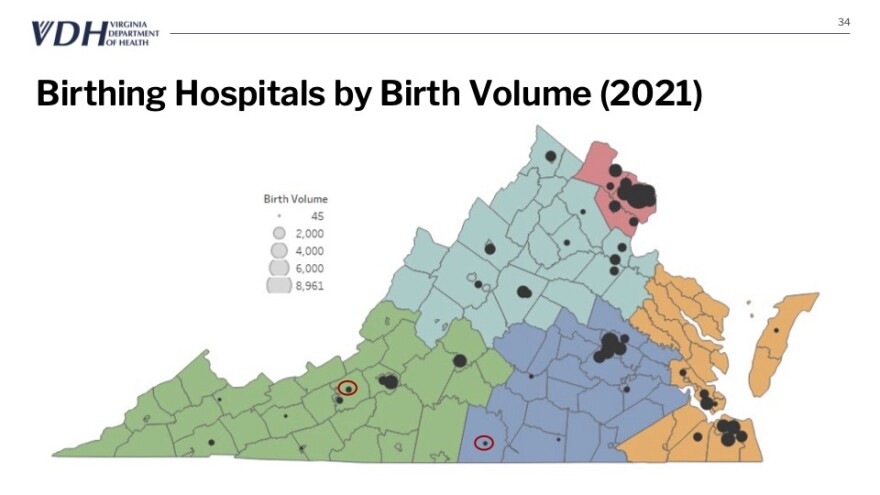
A 2020 study out of North Carolina found closures of rural labor and delivery units have increased the rate of induced labors. And a late-2023 national study found that people in maternity care deserts experience preterm births at significantly higher rates.
“We got to the induction date,” Cassidy said. “The day before the induction, I went into labor on my own.”
She had been having what she thought were false contractions all day, but didn’t want to make the drive only to be turned away because she was too early in her labor. By nighttime, her contractions had settled into 10–15 minute intervals and she decided to take a shower.
“I got in the shower, got out of the shower and my water broke,” she said. “After my water broke, the contractions were five minutes apart — we left the house 10 minutes after I got out of that shower.”
When Cassidy and Wallace passed Front Royal — where Warren Memorial Hospital’s labor and delivery unit used to be — her contractions were less than 5 minutes apart.
“This whole scenario of ‘We're gonna have this baby on the side of the road’ was a very strong possibility,” Cassidy recalled. “This is what we didn't want. But luckily it was at nighttime, and we didn't hit traffic.”
They made it to Winchester Medical Center, where she delivered her son, Colton. Cassidy said his delivery was the “best” of her three, largely because of the care, respect and attention Valley Health staff provided.
But she knows making it to the hospital was partially due to luck.
“He could have just been situated just a degree to the left that was preventing him from just getting into your hips,” she said. “We could have just gotten lucky that that's the reason why he wasn't born on the side of the road.”
Nurse Jennifer Baugher has worked at Sentara in Harrisonburg for 24 years and is the team coordinator at the Family Birthplace unit.
Baugher sees patients from Page County and will occasionally see people from as far as Highland County or even West Virginia — at least a 50-minute drive over Shenandoah Mountain, in ideal conditions.
“Sometimes they're arriving here pretty advanced in their labor,” she said. “Others may not make it to the hospital before they deliver, so they might need to utilize emergency medical services to come by ambulance or they may have to pull off the side of the road.”
According to Baugher, she sees “maybe a handful, if that, a year” who deliver on the side of the road or at businesses along the way.

How maternity care deserts risk pregnant people’s health
About a year after Fallon Brumback’s second pregnancy almost killed her and her newborn, the family relocated from Northern Virginia to Luray, the seat of Page County.
The former government contractor had always wanted three children, but the delivery experience shook her and she started birth control. The family moved out to the Page Valley in 2012 to live in her husband, Edward’s, hometown — and life was normal until 2017.
“I don't know why I took the test. Just something told me to take the test,” she said. “When it came back positive, I absolutely panicked.”
After her first thought — “I need to find a doctor and I don't know where to find one” — Brumback’s attention shifted to how a Page County pregnancy would work. Fairfax County, where she had lived before, has the most doctors of anywhere in Virginia and is surrounded by some of the commonwealth’s best hospitals, according to US News and World Report.
While Page County does have a hospital with an emergency room — Page Memorial in Luray — the facility does not offer obstetrics care or a labor and delivery unit. Cassidy said she was able to receive basic pregnancy care there once, but was turned away when she went back with minor complications.
“The second time I went, it was basically ‘We're not labor and delivery,’ they basically recommend to go to a hospital that had labor and delivery,” she said. “I wasn't in risk of going into labor, but there wasn't a whole lot that they could do without having labor and delivery.”

She said there were two episodes where she experienced worrying symptoms — “I know my blood pressure is dropping, and I can't get it to go back up no matter what I do” — but didn’t go to the hospital for treatment.
“We would have to pack the older two kids up and then drive an hour to the nearest hospital that would actually take me and help me if there was an emergency,” she said. “I mean [Page Memorial is] 10 minutes down the road; I'm sure they would figure it out if it was an absolute emergency, but knowing that they don't have the capacity, they don't have the doctors and nurses that are specifically trained for it, I mean, it's a little bit uneasy.”
EMT Kourtney Minton said the woman she helped deliver had stopped at Page Memorial before unsuccessfully trying to make the drive to Sentara in Harrisonburg.
Valley Health operates hospitals in Page County, Shenandoah County, Front Royal, Winchester and two in West Virginia.
In a statement to VPM News/WMRA, Chief Physician Executive Dr. Iyad Sabbagh for the health system’s Valley Physician Enterprise did not directly address questions about turning pregnant patients away from Page Memorial.
He did note that “even though we don’t deliver babies in these smaller hospitals, we do offer prenatal care in each of these locations.” As of June 25, none of the system’s six hospitals list “prenatal care” as an offered service on their respective Valley Health webpages.
“I remember being concerned about ice on the mountain having to drive to Warrenton at night, alone ... and the rational-irrational fear that ‘I'm going to have to pull over and have this baby.’”
Brumback had a lot to consider to pick where she would deliver: She had gone into preterm labor twice already, she would likely have to travel back and forth to the hospital, she might need to make the drive while in labor — and the family would need child care for the two children who would have to stay at home.
In the end, she chose Fauquier Health in Warrenton — a nearly hour-long drive away — because her husband worked near there.
Midway through her third trimester, except for gestational diabetes, the pregnancy was going smoother than her first two. Because of her second pregnancy’s complications, Brumback chose to schedule a cesarean section delivery. While she said the choice was a relief, it didn’t provide total peace.
“But in the back of your mind, you're still like, 'Well, what happens if I do go into labor?' And then the complications with the time of day and whether or not the kids will be home,” she worried. “And can I make the drive in active labor to the hospital? And, if not, is there time for my husband to drive the hour home and then us drive another hour back to the hospital?”
A full-term pregnancy is about 40 weeks; anything before 37 weeks is considered preterm by federal and state health agencies.
At about 36 weeks, Brumback started experiencing contractions late one night. With her husband needed at home to care for their young children, Brumback started the nearly hour-long drive over the Blue Ridge Mountains to Fauquier Health.
“I remember being concerned about ice on the mountain having to drive to Warrenton at night, alone, on possibly treacherous roads, while having these contractions,” she said. “And the rational-irrational fear that ‘I'm going to have to pull over and have this baby.’”
On top of that, she worried about a worse outcome.

“And then the fear of: ‘I'm having contractions, they hurt, it's late, I'm tired, the roads are not safe.’ If I'm going to run off the road — something horrible is going to happen,” she said.
As she crossed the mountains, Brumback repeated a mantra: “Just get there, just get there, just get there.”
She did and the contractions ended up being a false start. But, one week later at a routine appointment, doctors found she had HELLP Syndrome — a rare but life-threatening complication where a person’s red blood cells start to break down and their liver begins to fail. It can lead to excessive bleeding, liver rupture, strokes and more.
While her husband frantically arranged child care back home, Brumback was whisked to the operating room.
“The doctor came in, took one look at me and said, ‘OK, we're having a baby,’” she recalled. “10–15 minutes later, I was in a hospital bed with needles going in and an operating room being prepped. I think the total time from her telling us that to the baby being born was maybe 45 minutes.”
Her daughter, Abigail, who is now 6, was born healthy and Brumback recovered but the birth process almost killed her — again. Thinking back now, she feels certain she would have died if she hadn’t made it to the hospital or had given birth back in Page County.

According to Baugher, who runs Sentara’s labor and delivery unit, situations like Brumback’s get at the heart of why limited access to prenatal care is life-threatening.
At her unit, Baugher said if a pregnant person is bleeding profusely or a baby gets stuck during delivery, they have access to OB/GYN physicians 24/7 as well as nurses with decades of experience.
“If you don't have those staff, those personnel, at the side of the road or in the back of the ambulance,” she said, “it does present a risk, because there's no one who is trained in that type of emergent care.”
VPM News/WMRA spoke with four of Sentara’s Family Birthplace nurses. None had seen issues like these lead to a pregnant person’s death.
That’s not surprising, because maternal mortality is generally rare.
95,618 babies were born in the commonwealth in 2021, the most recent year the Virginia Department of Health has maternal mortality data for. Out of those, 64 birthing people died either while pregnant or in the year after.
But maternity care deserts do contribute to pregnant Virginians' deaths.
Melanie Rouse holds a Ph.D in health services research and is VDH’s maternal mortality programs manager. As a part of that job, she coordinates the Virginia Maternal Mortality Review Team — a group charged with reviewing every death of a Virginia resident who was pregnant at the time of death or died within one year of the end of a pregnancy.
Rouse said her team has reviewed cases where a lack of access to care or a lack of access to higher-level care “did contribute to the death.”
“It is a regular contributor,” she said. ”It is one of our top contributors that we do see — particularly in cases in the rural areas.”
Additionally, Rouse said people of color — especially Black women — are disproportionately impacted.
“In urban areas, those rates can be two to three times as high among Black women when compared to other races,” she said. “Whereas in rural areas, the disparities tend to be a little bit closer together; particularly because, when you think about it, in general, all women in those areas are dealing with the same access issue to an extent.”
Katherine Schroeder is the population health manager for Lord Fairfax Health District, which oversees public health in Page County.
She said that because the county is so white — all but 4.9% of the population — it can be hard to talk about any potential disparities because adding information like race and time frame to data can effectively de-anonymize it.
Of Virginia’s more than 130 counties and independent cities, CDC WONDER data on deaths by county is only available for five — Chesterfield, Fairfax, Henrico and Prince William counties as well as the city of Norfolk.
But, with 15 deaths in 2021, the Northwestern Health Services Area — which includes the Shenandoah Valley — had the highest rate of pregnancy-associated deaths at 101.1 deaths per 100,000 live births, according to the 2024 Virginia Maternal Mortality Review Team Annual Report.
(NHSA is composed of 32 counties in the commonwealth’s northern and western regions, excluding Northern Virginia. The southern half of the Shenandoah Valley appears to have the highest death rate in NHSA, according to the Virginia Department of Health’s 2023 report.)
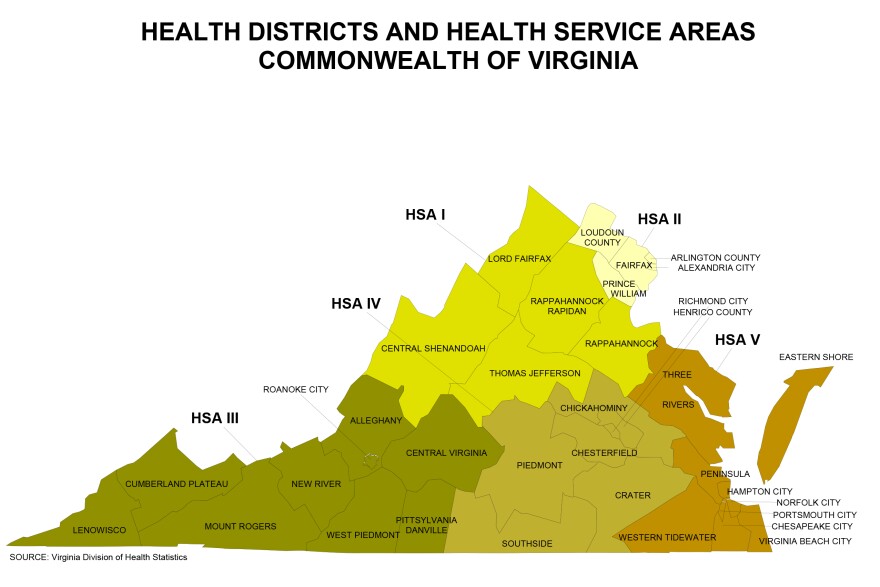
While county-level data on deaths and disparities is not available, trends in the commonwealth at large are clearer.
Virginia’s maternal mortality rate more than doubled between 2019 and 2021, according to a 2023 investigation from the Virginia Center for Investigative Journalism.
Fifty-three people died in pregnancy-associated deaths in 2019, according to the most recent Virginia Maternal Mortality Review Team Annual Report. Eighty-two people died in 2020. And 64 people died in 2021.
National CDC data released in May showed maternal mortality rates had lowered back to pre-pandemic rates — 19 maternal deaths for every 100,000 live births — by the end of 2023.
Data on Virginia’s rate is not available beyond 2021 but the commonwealth’s has consistently been higher than the U.S. rate, often by a factor of more than two.
A growing problem
Nearly one-third of Virginia counties are maternity care deserts.
While the rate of OB/GYNs per woman in Virginia — 12.84 per 100,000 — puts it in the top third of U.S. states and territories, 59 of Virginia’s 133 counties and independent cities have no OB/GYN, Health Resources & Services Administration data shows.
In the Shenandoah Valley, Page County, Lexington and Buena Vista all lack active OB/GYNs. Fourteen other Virginia localities have only one active OB/GYN, including Staunton and Warren County.
Since Warren Memorial closed its labor and delivery unit in 2018, VPM News/WMRA found three other hospitals have closed their units: Sovah Health-Martinsville in 2022, Sentara Halifax Regional Hospital in 2023 and Blacksburg’s LewisGale Montgomery earlier this year.
On top of increasing the distance pregnant people have to drive to get care and give birth at hospitals, research has found these closures can increase the rate of severe maternal morbidity — a medical research term for serious, potentially life-threatening maternal health problems — especially for Black and Hispanic women.
In his statement to VPM News/WMRA, Valley Health’s Dr. Iyad Sabbagh said low demand was the reason for the closure of Warren Memorial’s L&D unit.
“In smaller communities, the need for many specialties, such as obstetrics, neurosurgery, cardiology are not great enough,” he said, “nor required frequently enough for those physicians and staff to remain competent and experienced in providing those services.”
Instead, the health system has centralized services in larger hospitals like Winchester Medical Center. Sabbagh said this helps retain staff and increases the quality of care.
“In smaller communities, the need for many specialties, such as obstetrics, neurosurgery, cardiology are not great enough...”
Baugher, of Sentara, said that operating obstetric practices is increasingly expensive and difficult, especially for independent operations that can’t negotiate good prices for materials because of smaller purchase sizes.
Because of this, she said the trend of closures will likely continue.
“Unfortunately, what we're seeing is it's probably going to continue that direction unless there is something that comes about through the government that's going to help,” she said, “either subsidize the smaller hospitals to help them to be able to maintain obstetric services and maternity care or to create more clinics.”
Those are unlikely with a divided Congress that has shown increasing hostility to social protections and public health, and a presidential election only months away.
Rouse said that while COVID-19 and its impacts on our health care system aggravated these problems, they will only continue to worsen without action. But she said that there has been some action on the issue in recent years.
“One of the good things that we've done as a state is implement that Doula reimbursement through Medicaid,” she said, “and also the legislation has passed for private insurance to reimburse doulas.”
Rouse also pointed to the specialized and local care that midwives, home visiting programs and some community-based organizations provide as solutions to address care deserts and their impacts on pregnant people.
But, for people in the areas without access to care, the issue is urgent.

Jayne Michaud is a pregnant mom of two in Luray. After bouncing around the country while growing up in a military family, she landed in Florida. There, she met her now-husband and delivered their first child 10 minutes down the road from where they lived.
Michaud was six months pregnant with their second child when they moved to the rural, far northwestern part of Shenandoah County. She was shocked to find it would take more than 50 minutes to get to the nearest birthing hospital.
“I was Googling like ‘Rural maternal health care solutions’ and then it will bring you to different government websites,” she said. “And then they'll say ‘Contact us if you have any concerns, [are] looking for programs in your area,’ all of that good stuff.”
But, as of late March, Michaud hadn’t heard back from any.
Her experience helps illustrate the reality for many pregnant people in rural areas: in theory, health systems and government bodies like health departments have mandates to provide obstetrics care in rural areas but, in practice, the care is often simply not there.
Schroeder, the health district’s population health manager responsible, said that while the Virginia Department of Health mandate requires all localities be covered by a health department, the services they’re able to provide are limited.
“Even though we recognize that there is a need for it, the health department isn't quite set up to open a labor and delivery unit as much as it may be needed,” she said. “But we have a number of programs that do support, whether indirectly or [directly, people where] we can impact health outcomes and provide better opportunities.
She pointed to the national supplemental nutrition program for Women Infants and Children, family planning services and programs that help people quit smoking. Schroeder said LFHD’s services are oriented toward population centers like Winchester — and rural areas like Page County develop safety net services themselves.
“Oftentimes, the people who live in Page County, they figure out their own way to support their community members,” she said. “So there's a lot of local organizations who focus on one specific niche and one specific concern, and they provide that one service or those few services in order to kind of fill the gap that's been left.”
For obstetrics, the closest thing to that in Page County is one OB/GYN who comes to the county’s free clinic once a month.
Cassidy, the Rileyville mom who barely made it to the Winchester Medical Center before delivering, said that reality leads to a culture of home births.
“The area around here… it was just so common and just a general knowledge of ‘You just have babies at home,’ that it's just so embedded,” she said. “But there's plenty of people that grew up with that, that just don't want that option or feel like they have to because there is no other option.”
She and her boyfriend are seriously considering having one or maybe two more children, and she said they plan to try driving to Winchester again if they do.
“I don't really have any other other choice, my neighbor has not convinced me to have a home birth. She jokingly mentioned that she still had her home [delivery] bag,” Cassidy said. “She's like, ‘Well, it's still over here if you go into labor, we can just have this baby at home.’ But we'll probably just do the same thing.”

Michaud, the pregnant mom of two in Luray, switched from Sentara to a midwife at Brookhaven Birth Center for her current pregnancy. She said it’s cheaper, offers a less restrictive birth environment and the midwife would come to her house if she couldn't make the 45-minute drive to Harrisonburg.
“I'm gonna get in the car and go,” she said of her delivery plan. “And if it feels like 20 minutes down the road I'm not going to make it, I'm to turn around and go back to my house.”
The plan, the fact her deliveries have gone well and the option for the midwife to come to her have calmed some of her anxieties.
“Women have been having babies for thousands of years,” she said, audibly making peace with a potential home birth. “And if you have to have a bathtub baby because your rural health care is that crappy, then you gotta have a bathtub baby.”
But her worries about a possible car birth have only intensified. As short as her first labor was, her second was even shorter. Multiple times a day, she gets nervous thinking about what could happen if she can’t make it to Harrisonburg or back home.
“I don't want to have a car baby. And if something goes wrong with me while I'm having this car baby, it's just another issue,” she said. “And I think I'm gonna have the car baby. Like, in my mind, there's no other option other than to have my baby in a car because I can't make it to the hospital.”
Michaud is due Oct. 17.
Editor's note: Sentara RMH Medical Center and the Virginia Department of Health are VPM News sponsors.




